From First Effort to Best Effort
The Essentials
There are some essential techniques, tricks, and adjuncts you can learn and use that will DRAMATICALLY improve your ability to oxygenate your patients with a BVM.
Study and practice these FVM optimization strategies carefully.

Click here to open a full-sized image in a new tab.

MANIPULATIONS
Optimization of Face-Mask-Ventilation – and every other lifeline for that matter – begins the same way every time: fundamental airway manipulation.
There are 2 core manipulation techniques that instantly open the airway in an unresponsive, apneic patient. These maneuvers reposition the patient and make anatomy work for you, not against you. You should perform them in every patient who is hypoxic, even before reaching for any of the three lifelines. They are:
- Jaw Thrust
- Head-Tilt, Chin-Lift
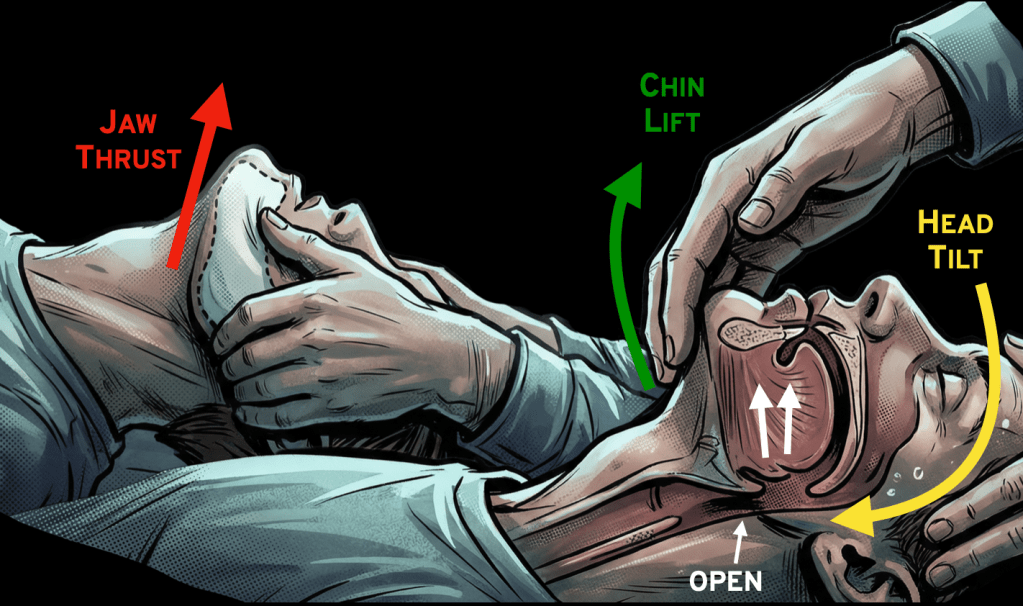
Jaw Thrust
The jaw thrust maneuver involves placing your thumbs and thenar eminences over the patient’s cheekbones and using the other eight fingers to reach behind the angle of the mandible to displace the entire jaw forward (creating an underbite).
Yes, just like the vice grip, but without the face mask.
This lifts all the structures of the anterior airway (tongue, epiglottis, muscles, fat) away from the posterior oropharynx creating an unobstructed passageway for air.
Check out this brief video from the NEJM that shows just how dramatic of an impact the jaw thrust maneuver has.
Fun Tip: forcing the mandible forward with your hands can be quite painful (try on yourself). While this wouldn’t be very nice to an awake patient, performing a jaw thrust in a patient who is unexpectedly found to be unresponsive kills three birds with one stone: 1) it opens the airway, and 2) allows you assess the patient’s level of responsiveness to pain, and 3) triggers the patient to wake up and take a breath. This can be very helpful in a patient who is intoxicated with a CNS depressant (opioid, EtOH).
Head-Tilt, Chin-Lift
Just like the jaw thrust, this maneuver works by displacing the structures of the anterior airway away from the posterior oropharynx. Just by tilting your head back and lifting the chin, the airway becomes more patent. Try on yourself: touch your chin to your chest and take a breath, then tilt your head back and take a breath. Can you see the difference?
This quick video shows you how to perform the head-tilt, chin-lift maneuver:
This is key to face mask ventilation. Whether you’re performing the one-person or the two-person technique, the head-tilt, chin-lift maneuver will significantly improve your ventilation.
Caution: avoid the head-tilt, chin-lift maneuver if you suspect that your patient may have a c-spine injury!! In this case, the jaw thrust maneuver is preferred. This will usually require more than one pairs of hands: someone to hold c-spine, someone to hold mask & jaw thrust (vice grip), and someone to bag.
Adapting to Facial Variation
No two patients are the same. Facial hair, dentures, facial structure, age-related changes, and prior surgery can all influence the effectiveness of face-mask ventilation. Providing high-quality, equitable care requires recognizing these normal variations and understanding how to adjust your technique accordingly. Let’s take a moment to review two common clinical presentations you almost guaranteed to encounter and the specific modifications that optimize mask seal and ventilation.
Dentures
If you never thought about what you would do if you were bagging a patient with dentures, if you never made a plan for this specific scenario, your instinct might be to consider dentures a foreign body and get rid of them immediately.
And you’d be correct for 2 out of 3 airway lifelines. Unfortunately, not for FMV.
While removing all obstacles is preferred for endotracheal intubation or the placement of a supraglottic airway, an effective mask seal depends on the structural fullness of the face. Dentures help maintain facial contour and provide a stable surface against which the mask cushion can seat. When dentures are removed, the loss of support can lead to inward collapse of the cheeks and lips, increasing air leak and making ventilation more difficult. Hence the mnemonic:
“BAG IN, TUBE OUT”
Bag refers to BVM and tube refers to ETT (or SGA).

Beard
Facial hair disrupts the contact between the mask cushion and the skin, allowing air to escape and making it harder to generate adequate tidal volumes. Unlike dentures, this is not about structural support. It is about seal integrity.
To compensate, you must improve the seal. Strategies include applying water-soluble gel to the beard to reduce air leak, or using a large piece of occlusive transparent dressing (e.g. Tegaderm ®) to cover the facial hair and cutting/poking a hole for ventilation.

ADJUNCTS
Perhaps more than any other lifeline, face-mask ventilation can be significantly improved with three very simple, yet very powerful adjuncts:

In a nutshell, the first two help bypass or displace upper airway anatomy and decrease airflow resistance. The third adds resistance at the exhalation port of the BVM, and thus increases the pressure against which the patient exhales (PEEP) allowing the alveoli to remain filled and oxygenated.
Because of how powerful these three adjuncts are, they will be covered in depth in the next three stations of the FMV section.

SIZE & TYPE OF DEVICE
Choosing the right mask size and optimizing how it sits on the face can dramatically improve your ability to oxygenate.
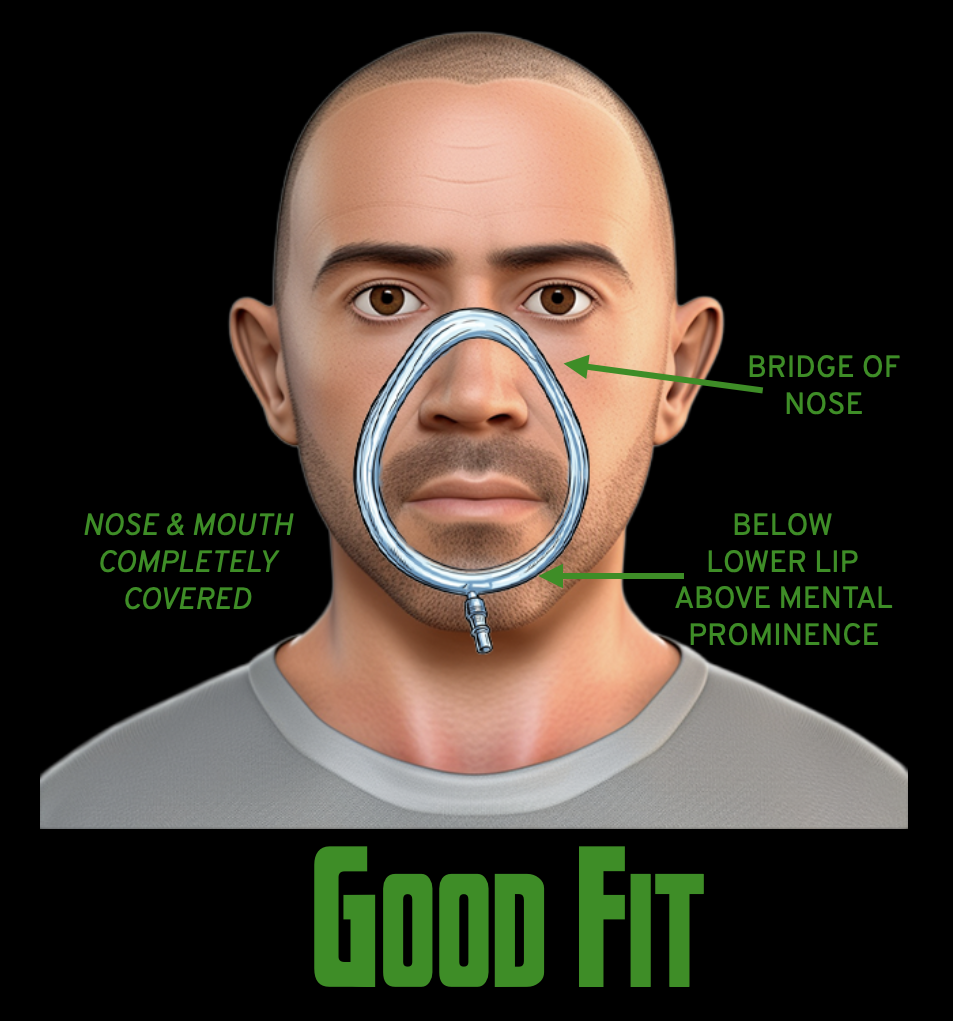
A properly sized mask will rest on the patient’s nasal bridge superiorly, cover the nose and the entire mouth, and rest in the crease just above the mental prominence inferiorly.
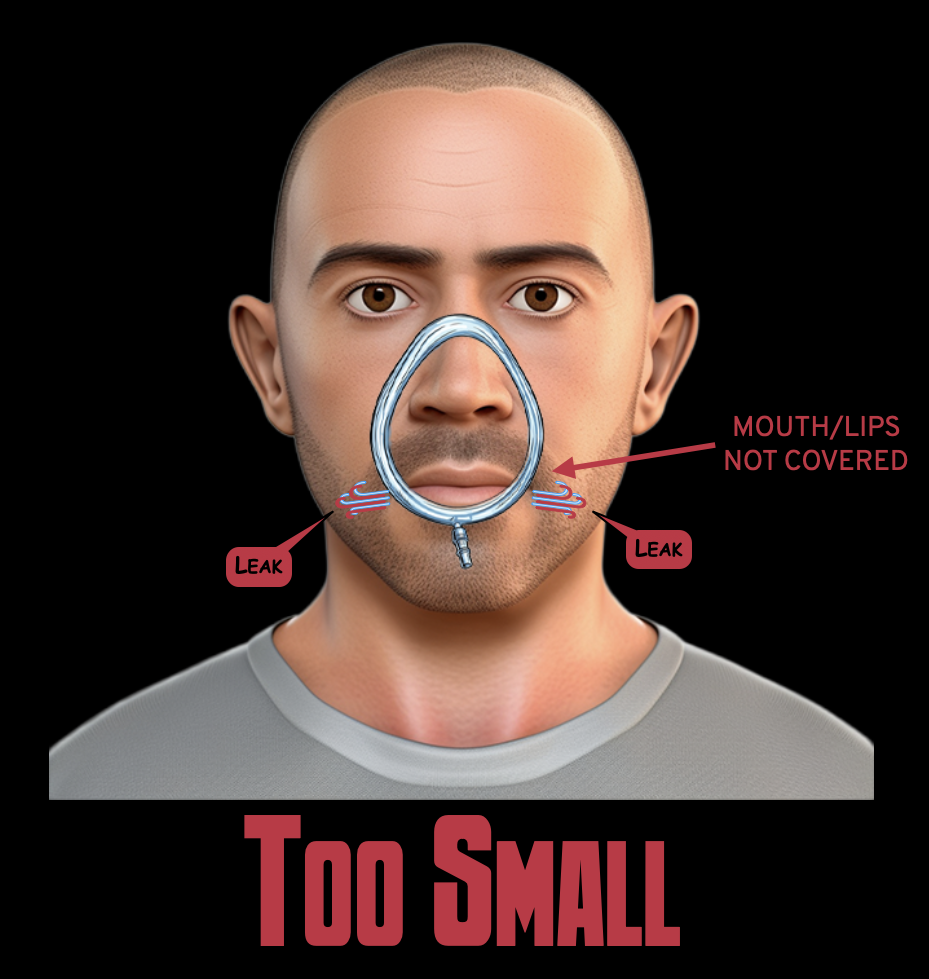
A mask that is too small will fail to cover the lips properly, and allow the air to leak inferiorly:
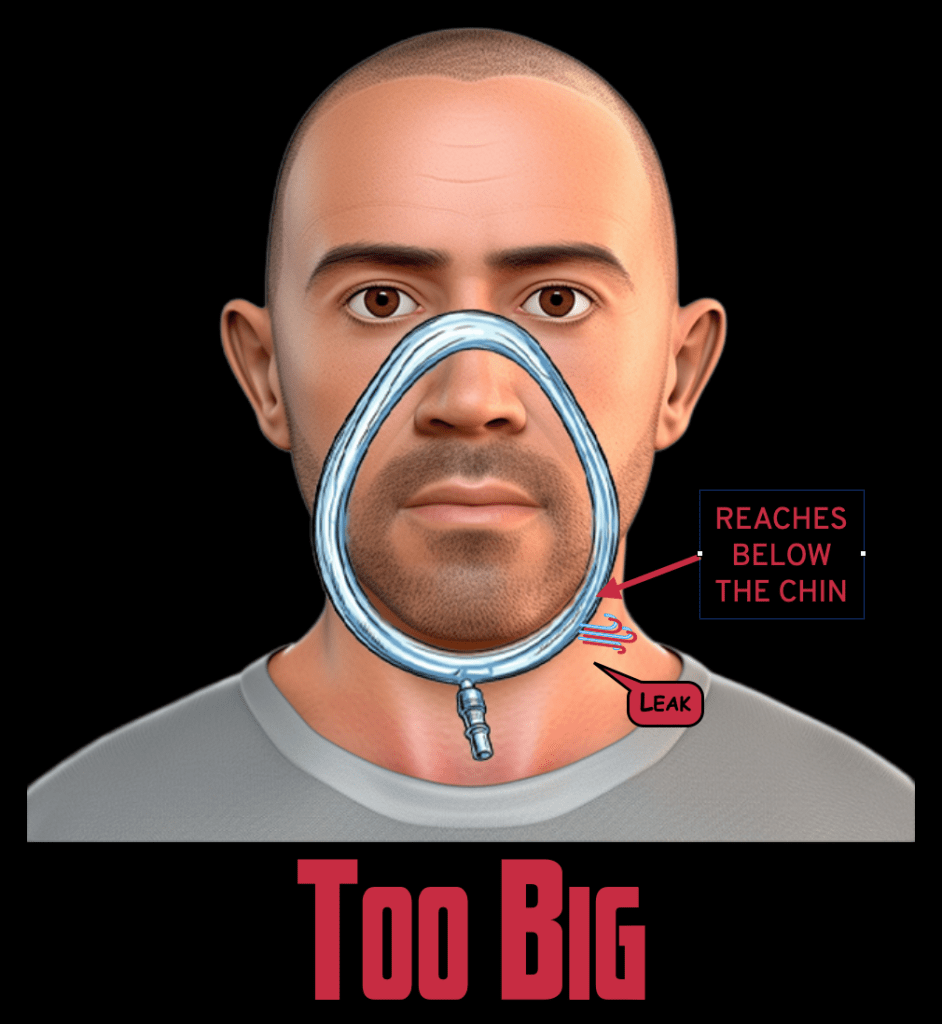
Conversely, a mask that is too big will either extend below the chin causing a leak inferiorly, or it will sit over the orbits/eyes and lose seal superiorly:

🎧 Deep Cuts
We like to showcase other great educators to help you build your learning network by curating online resources.
Here is another excellent segment by Dr. Lahiru Amaratunge from his YouTube channel, “The ABCs of Anesthesia”.
Title: “The Beginners Guide to Bag Mask Ventilation | Essential tips and tricks to ventilate your patient” Start: 2:17 – End: 3:02 – Total Length: 0:45.

SUCTION & O2 FLOW
Let’s get one thing straight… you are never truly prepared for managing an airway if you do not have oxygen and suction! They are the first two things you reach for as a critical patient arrives.
In fact, if there is only one thing you take home from today’s lesson, let it be this:
YOU SHALL NEVER MANAGE AN AIRWAY WITHOUT OXYGEN OR WITHOUT SUCTION.
This goes beyond optimization of FMV. Oxygen and suction are the foundation. They are the beginning.
Oxygen
But why mention oxygen as an optimization strategy? Isn’t it obvious? The answer is simple: stress & cognitive bandwidth.
It may seem obvious when you’re relaxed, reading, or practicing with manikins. But when you’re full of adrenaline during a resuscitation, simple things get overlooked. Building oxygen into the vortex approach under the framework of optimization is a powerful, and lifesaving, reminder.

Suction
Blood? Saliva? Emesis? The type of contamination is irrelevant. What is relevant, however, is that it will prevent you from properly oxygenating your patient. What can you do? Suction! Suction early. Suction aggressively. Suction frequently. A clear, decontaminated airway = increased success with every single lifeline.

MUSCLE TONE
As the final category of optimization strategies recommended by the Vortex Approach, “Muscle Tone” is consistent and relevant across all three lifelines, not just FMV.
It refers to pharmacologic sedation & paralysis, used in general anesthesia and rapid sequence induction.
While the process of RSI and the pharmacology of sedatives and paralytics are beyond the scope of this installation, the bottom line is this: the more awake, tense, and agitated your patient is, the more difficult it will be to ventilate them.
Sedation reduces protective reflexes and neuromuscular blockade (paralysis) eliminates active airway resistance and muscle opposition. Jaw tension resolves, vocal cords relax, and chest wall compliance improves. With no competing spontaneous effort, positive pressure ventilation becomes more controlled and efficient. The goal is to work for the patient, not against them.

If you want to dive deeper into the process of RSI and airway pharmacology, you can visit our dedicated learning spaces by clicking the buttons below and purchasing full access to our content.
What’s Next
Find Or Click Me
Nice work! To keep going, visit the next poster in our pop-up training space, or continue online by clicking the poster here.
Follow Us





You must be logged in to post a comment.