NextGen Learning To Elevate Your Airway Practice
Overview
A Step-by-Step Approach to the Difficult Pediatric Airway
Managing a difficult pediatric airway is one of the most high-stakes challenges in emergency and critical care medicine. Kids aren’t just “small adults” when it comes to airway anatomy and physiology—smaller airways, a higher and more anterior larynx, and a greater risk of desaturation all make intubation trickier. That’s why having a clear, step-by-step plan is essential, from recognizing risk factors and optimizing preoxygenation to choosing the right tools and knowing your backup strategies. In this guide, we’ll walk through a practical, evidence-based approach to handling a difficult airway in a pediatric patient, ensuring you’re prepared to act decisively and safely when it matters most.
1. Anticipate & Assess the Difficult Airway
Managing a difficult pediatric airway requires meticulous planning, preparation, and execution to optimize success and minimize complications. Below is a stepwise, evidence-based approach from current pediatric airway management guidelines.
Perform an airway assessment:
- MOANS (for BMV difficulty): Mask seal, Obstruction, Age (<1 yr), No teeth, Stiff lungs
- LEMON (for laryngoscopy difficulty): Look externally, Evaluate the 3-2-1 rule, Mallampati (if possible), Obstruction, Neck mobility
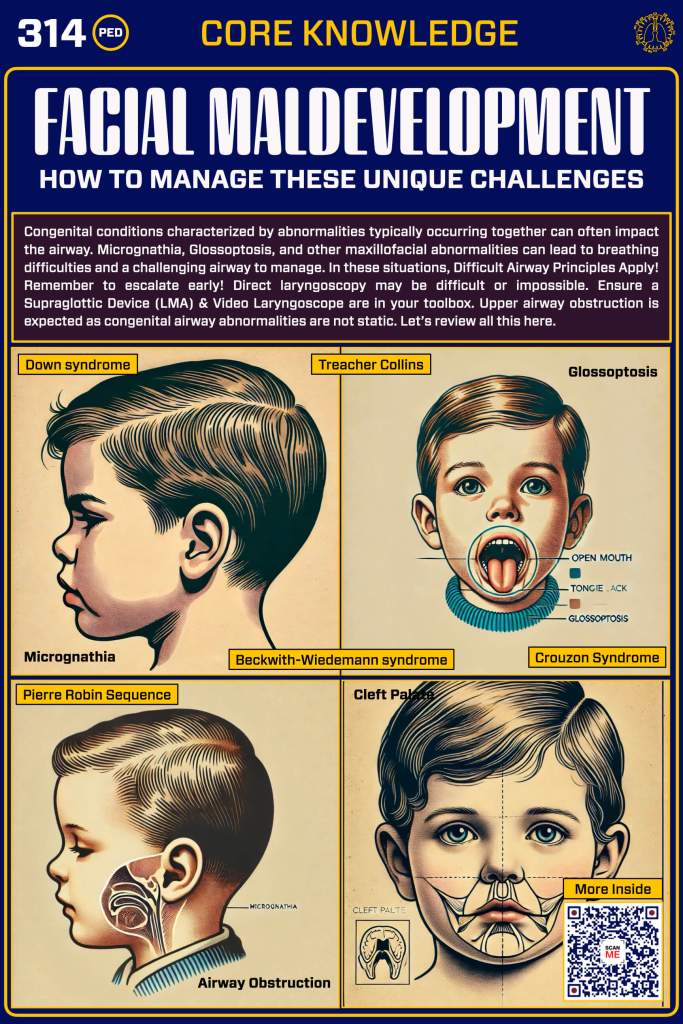
- Pediatric-specific predictors: Micrognathia, Pierre Robin sequence, Treacher Collins syndrome, large tongue, high anterior larynx, subglottic stenosis
Stratify risk level:
- Difficult mask ventilation but easy intubation? → Optimize BMV technique
- Difficult intubation but easy ventilation? → Consider awake techniques
- Difficult ventilation + difficult intubation? → Prepare for an emergency surgical airway
2. Optimize Patient & Environment
Team communication & roles:
- Assign key roles
- Discuss your plan for intubation, backup, and escalation
- Use closed-loop communication
Positioning:
- Infants: Shoulder roll to align external auditory meatus with the sternal notch
- Older children: Sniffing position if no contraindications
- Obese patients: Ramped position for optimal alignment
Preoxygenation:
- High-flow nasal cannula (HFNC) or bag-mask ventilation (BMV) with PEEP
- Consider non-invasive ventilation (NIV) or CPAP for high-risk patients
- Apneic Oxygenation with nasal cannula at 15 L/min during laryngoscopy
Hemodynamic stability:
- Optimize volume status, consider push-dose epinephrine (1-2 mcg/kg IV) for hypotension

3. Prepare Your Equipment & Backup Plans
Airway Cart Setup: “Plan A, B, C, D”
- Plan A (First attempt – Best effort first!)
✅ Video laryngoscopy (VL) as the first-line device (pediatric studies support increased success)
✅ Age-appropriate endotracheal tube (ETT) – cuffed tubes preferred
✅ Bougie or stylet-assisted intubation - Plan B (Alternative device or technique if first attempt fails)
✅ Second VL attempt (optimize head positioning, suction, BURP maneuver)
✅ Consider different blade size (Miller for neonates, Mac for older kids)
✅ Consider fiberoptic-guided intubation via supraglottic airway (SGA) if available - Plan C (Rescue oxygenation if multiple failed intubation attempts)
✅ Supraglottic airway (LMA/i-gel) for ventilation
✅ Optimize mask ventilation techniques - Plan D (Can’t intubate, can’t oxygenate – CICO scenario)
✅ Emergency front-of-neck access (FONA)
✅ Percutaneous cricothyrotomy (12+ years old) or needle cricothyrotomy (<12 years old)

Confirming Equipment Readiness:
- ETT cuff check, suction, VL/Direct laryngoscope light check
- Drugs drawn up & labeled (see below)
- CO₂ detector and ventilator ready
4. Choose Optimal Pharmacologic Agents
Induction Agents:
- Ketamine (1-2 mg/kg IV) – preferred for hemodynamic instability
- Propofol (1-2 mg/kg IV) – for normotensive patients
- Etomidate (0.2-0.3 mg/kg IV) – stable but may suppress adrenal function
Paralytic Choice:
- Rocuronium (1.2 mg/kg IV) – longer-acting, ideal for difficult airways
- Succinylcholine (2 mg/kg IV) – rapid onset, shorter duration but contraindicated in neuromuscular disease, hyperkalemia
Adjuncts:
- Atropine (0.02 mg/kg IV, min 0.1 mg) for bradycardia in infants
- Lidocaine (1 mg/kg IV) for suspected raised ICP
5. Perform the Intubation
Best First Attempt Strategy:
- Optimize visualization: Use VL (preferred in difficult cases)
- Bougie-assisted intubation, if needed
- BURP (Backward-Upward-Rightward Pressure) or bimanual laryngoscopy
- Confirm placement: ETCO₂ detection (gold standard), bilateral breath sounds
If unsuccessful:
- Limit to ≤2 attempts before changing approach
- Reoxygenate before reattempting
- Move through the backup plans (B, C, D)
6. Post-Intubation Management
Confirm & Secure Tube:
- Capnography (ETCO₂)
- Chest rise, bilateral auscultation
- Tube depth confirmation (3 x ETT size in cm at lips for neonates, age-based formulas for older children)
- Secure ETT with tape or a commercial device
Ventilation & Sedation:
- Initial settings: PEEP 5 cmH₂O, tidal volume 6-8 mL/kg
- Maintain sedation & analgesia (fentanyl, midazolam, dexmedetomidine as needed)
7. Post-Procedure Considerations
Monitor for complications:
- Laryngospasm, bronchospasm, tube displacement
- Delayed airway swelling (e.g., post-extubation stridor → consider racemic epinephrine and steroids)
Summary Table: Quick Reference Guide
| Key Steps | Action Items |
| Assess Airway | MOANS, LEMON, Pediatric risk factors |
| Optimize Positioning | Sniffing position, ramped for obese children |
| Preoxygenation | HFNC, BMV with PEEP, nasal O₂ apneic oxygenation |
| Plan A: First Attempt | VL, cuffed ETT, bougie |
| Plan B: Alternate Approach | Change blade size, second VL attempt, fiberoptic |
| Plan C: Rescue Oxygenation | SGA, optimize BMV |
| Plan D: CICO Rescue | Cricothyrotomy (needle <12 yrs, scalpel >12 yrs) |
| Pharmacology | Ketamine, Rocuronium (preferred) |
| Confirm Success | ETCO₂, chest rise, breath sounds |
Key Takeaways
✅ Preparation and planning are critical – always have a stepwise approach
✅ Optimize first-pass success with video laryngoscopy and best attempt first
✅ Recognize failed attempts early and pivot to backup plans
✅ Confirm placement carefully and monitor for complications
The Bottom Line
Successfully managing a difficult pediatric airway requires a structured, evidence-based approach that prioritizes preparation, oxygenation, and first-pass success. Key steps include thorough airway assessment, optimal patient positioning, preoxygenation with strategies like HFNC or BMV with PEEP, and selecting the best equipment—often with video laryngoscopy and a bougie for difficult cases. Pharmacologic choices should support hemodynamic stability, and a clear escalation plan ensures smooth transitions through alternative techniques like supraglottic airways or fiberoptic-assisted intubation. Most importantly, recognizing failure early and having a well-rehearsed CICO (Can’t Intubate, Can’t Oxygenate) plan, including front-of-neck access, is critical to patient safety. By following a structured approach, you can improve outcomes and reduce complications in your pediatric airway cases.
Don’t Forget to Practice
Use this content for self-guided practice. When you’re comfortable with your initial progress, visit our expert faculty coaches for customized feedback. You can do this as many times as you like. This iterative practice and feedback process will take your skills to the next level.

Dive Deeper
Curated MedEd – If you have 40 minutes, listen to this comprehensive discussion by a seasoned clinician: Dr. Karen Wouters – Consultant Paediatric Anaesthetist & Difficult Airway Lead at Evelina London Children’s Hospital London, UK


You must be logged in to post a comment.