NextGen Learning To Elevate Your Airway Practice
Start Here
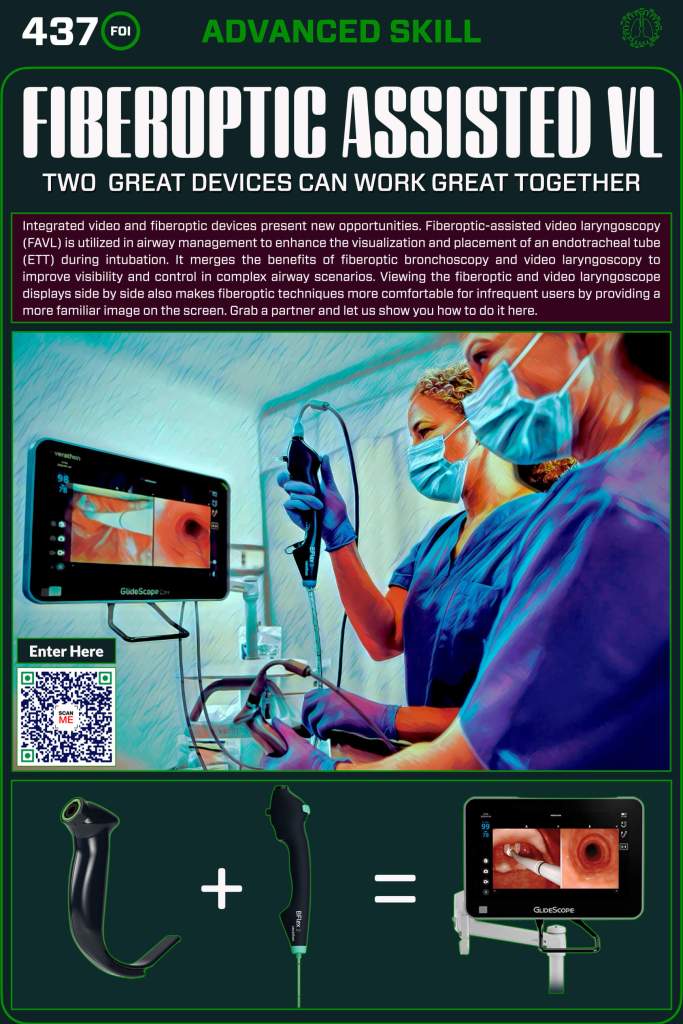
Video-Assisted Fiberoptic Intubation (VAFI)
Indication
Video-assisted Fiberoptic Intubation (VAFI) is indicated when traditional direct or video laryngoscopy is difficult or unsuccessful, particularly in patients with anticipated or encountered difficult airways. Specific indications include:
- Restricted mouth opening (e.g., temporomandibular joint disorders, facial trauma, post-radiation fibrosis)
- Distorted oropharyngeal anatomy (e.g., tumors, subglottic stenosis, or significant airway edema)
- Limited neck mobility (e.g., cervical spine immobilization due to trauma or disease)
- Failed direct or video laryngoscopy attempts
- Patients requiring awake intubation due to high aspiration risk, airway swelling, or difficult airway anatomy
Benefits
- Enhanced Visualization: Combines video laryngoscopy and fiberoptic bronchoscopy to optimize glottic visualization.
- Improved Tube Delivery: Video laryngoscopy provides a pathway, while fiberoptic bronchoscopy guides the ETT into the trachea.
- Increased First-Pass Success: Reduces airway trauma and repeated attempts, particularly in difficult cases.
- Useful in Awake Intubation: This can be performed under topical anesthesia in cooperative patients.
- Facilitates Team Coordination: The video screen allows Multiple providers to view the airway anatomy and intubation process.
Watch This
Step-by-Step Instructions for Performing VAFI
1. Preparation
Equipment Needed:
- Video laryngoscope (e.g., Macintosh or hyperangulated blade)
- Flexible fiberoptic bronchoscope (FOB)
- Endotracheal tube (ETT) (appropriately sized, preloaded over the fiberoptic scope)
- Suction setup
- Oxygenation tools (nasal cannula, high-flow O2, or supraglottic airway if needed)
- Lubricant for the fiberoptic scope
- Sedation & Airway Management Medications (if required)
- Local Anesthesia Supplies (if performing awake VAFI)
2. Patient Positioning
- Standard “sniffing” position if possible.
- If cervical spine precautions are needed, maintain neutral position with manual in-line stabilization (MILS).
- Nasotracheal vs. Oral Approach: Choose based on clinical need.
3. Airway Preparation (If Awake)
- Topicalize the airway with lidocaine spray (4%), nebulized lidocaine, or lidocaine-soaked gauze.
- Consider glycopyrrolate to reduce secretions.
- Light sedation (e.g., dexmedetomidine, remifentanil, or ketamine) may be used.
4. Video Laryngoscopy
- Insert the video laryngoscope and obtain the best possible view of the glottis.
- Optimize Blade Positioning: Avoid getting too close to the glottic opening, which could obscure the view.
5. Fiberoptic Scope Navigation
- Preload the ETT onto the fiberoptic scope.
- Insert the scope through the mouth (or nose, for nasal intubation).
- Guide the fiberoptic scope toward the glottis under video laryngoscopic visualization.
- Once the vocal cords and tracheal rings are seen, advance the fiberoptic scope into the trachea.
6. ETT Advancement
- While stabilizing the fiberoptic scope, gently advance the ETT over the scope into the trachea.
- Ensure correct placement by observing the carina or mainstem bronchi on the screen.
7. Confirmation of ETT Placement
- Withdraw the fiberoptic scope while confirming the correct positioning of the ETT.
- Use end-tidal CO₂ (capnography) and bilateral breath sounds to verify successful intubation.
- Secure the tube and reassess ventilation.
Key Pearls & Troubleshooting
- Fogging or Secretions? Use suction or warm the fiberoptic scope.
- Difficult Scope Navigation? Adjust the patient’s head, use jaw thrust, or reposition the video laryngoscope.
- ETT Gets Stuck? Rotate the tube 90° or adjust scope positioning.
- Unable to Advance Scope? Consider a supraglottic airway as a conduit for fiberoptic scope placement.
The Bottom Line
Integrating video laryngoscopy and fiberoptic bronchoscopy, VAFI improves visualization, enhances tube guidance, and increases first-pass success rates, making it a valuable technique in managing difficult airways.
This poster has associated hands-on learning opporunities in our immersive and interactive physical space. If you’re with us in person, please make sure to visit the related station and use the self-guided resources here.

Use the guided practice resources here to practice at your pace in a judgement-free zone. When you’re ready, visit one of our expert coaches for feedback on your technique.




You must be logged in to post a comment.